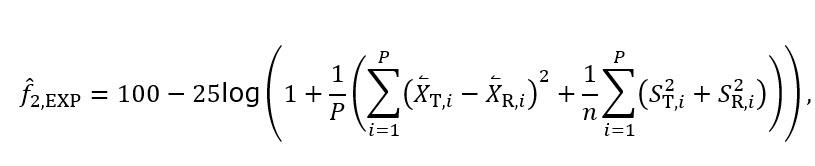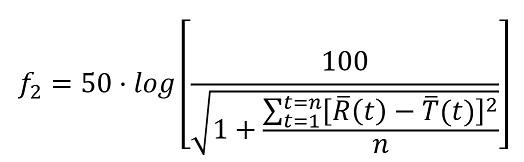Clinical pharmacology and pharmacokinetics: questions and answers
The questions and answers (Q&As) on this page provide an overview of the European Medicines Agency's (EMA) position on specific issues related to clinical pharmacology and pharmacokinetics.
HumanRegulatory and procedural guidanceResearch and developmentScientific guidelines